Poliomyelitis, better known as polio, is an infectious disease that was prevalent in the UK until a vaccine was discovered in 1950. The disease can cause flaccid paralysis if the virus enters the central nervous system. This paralysis may only be temporary and muscles are able to return to normal strength. However, if the paralysis is present 12 months following the infection, the paralysis is likely to be permanent.
For those people who do make a full recovery, there is a 25-50% risk of the individual developing similar symptoms of muscle weakness, or even new muscle weakness and extreme fatigue in adult life. This condition is described as post-polio syndrome (PPS). PPS is a progressive weakness for which there is no specific treatment. It is not, however, an infectious disease.
Because the first polio vaccinations were not introduced until 1955,post-polio syndrome is now becoming relatively common in patients who contracted polio in the 1940s and early 50s. According to the NHS that amounts to an estimated 120,000 people in the UK.
Minor symptoms of the poliovirus include flu-like symptoms, nausea and vomiting. When the virus enters the central nervous system, symptoms include fever, lethargy and extremity pain. Approximately five in 1,000 cases lead to symptoms of paralysis, where muscles in the extremities become weak and floppy.
Individuals suffering from post-polio syndrome will have had a previous diagnosis of polio, a long interval after recovery and onset of gradual weakness. The diagnosis can be confirmed by electromyography and imaging.
If a diagnosis is confirmed, then the patient will undergo a neurological examination. This includes: analysing joint ranges of movement; joint stability; muscle strength; standing posture/alignment; and a gait/walking assessment.
In PPS, people can develop symptoms after a long time, without any significant change in their condition, people may develop new symptoms of increasing weakness, stamina problems, fatigue and pain.
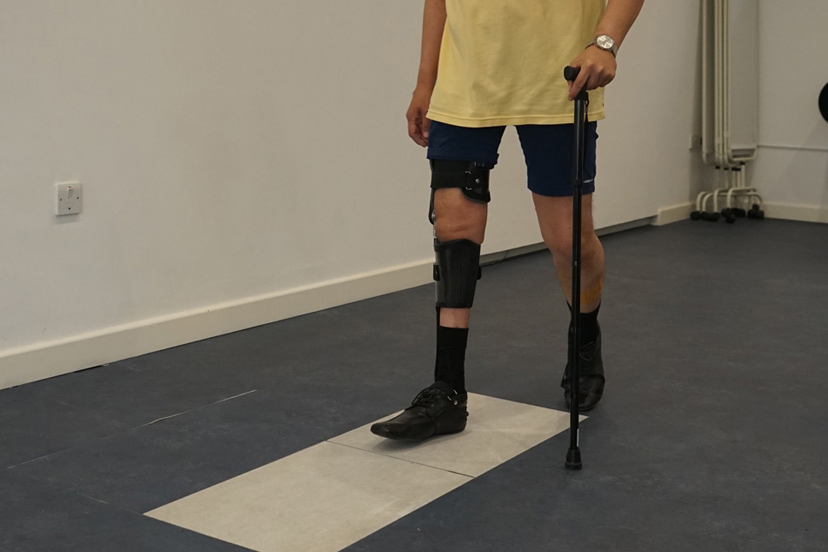
An individual with post-polio syndrome will suffer from muscle weakness and decreased mobility. Often they will be affected in areas that were not previously affected.
Commonly-used orthoses for treatment are ankle foot orthoses (AFOs) and knee ankle foot orthoses (KAFOs). These devices provide stability in stance and aid walking to improve energy efficiency and reduce pain. They are also designed to protect joints from abnormal forces.
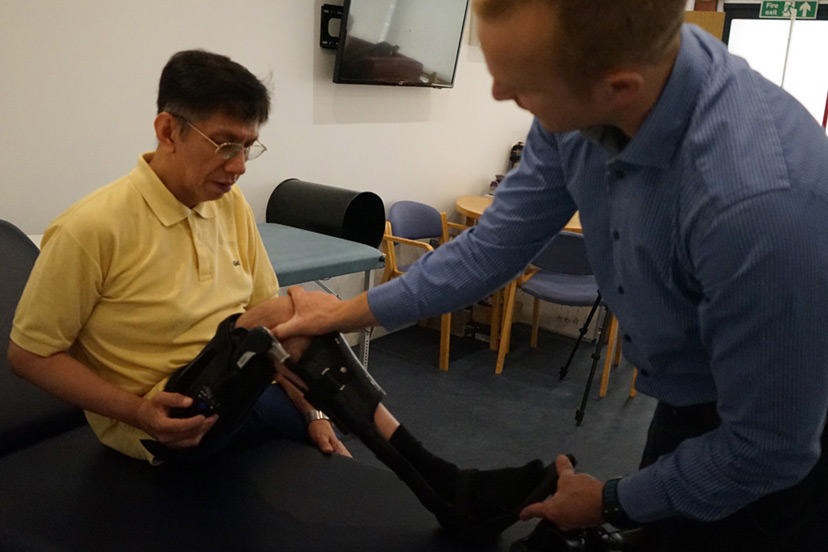
At LOC, we only fit bespoke ankle foot orthoses. These are designed and manufactured based specifically on the individual’s requirements, following a detailed assessment and casting.
We can manufacture traditional devices, but the more modern orthoses offer more leg control. They can also be made in lighter weight materials, such as titanium and carbon fibre. In comparison to traditional callipers, these modern orthoses are about a third of the weight. That is very significant. It both reduces strain on the patient and increases mobility. We have found the resulting reduction in weight a huge benefit to our PPS patients.
If desired, we can also make hybrid designs, keeping the familiar design and fitting characteristics of conventional KAFOs, but using the new lighter materials.


The British Polio Fellowship offers great support and assistance to people in the UK with the late effects of polio and PPS.
The Fellowship is able to provide direct grants to polio members towards their mobility needs this is particularly so for members in the Kingston and Wimbledon areas that close by to the LOC Head Office and Manufacturing Centre. For full details of the BPF grants and other assistance available and for membership enquires please contact the Fellowship directly:
[email protected]
Freephone: 0800 043 1935
01923 281 090
An AFO is an Ankle Foot Orthosis which as the name would suggest encompasses the ankle and foot. The objective is to control the position and movement of the ankle. AFOs are used to support weak limbs; they can also be used to immobilise the ankle and lower leg to correct foot drop. When set up correctly they can also have a great influence on the knee and hip joints. They are the most commonly used Orthoses.
The length of time that one needs to wear an AFO very much depends on the condition being treated. If it is a long-term condition like cerebral palsy or post-polio syndrome it is likely to be years as the condition cannot be cured. Your orthotist will advise you.
A patient’s comfort in their AFO is vital for compliance with the prescribed wearing regime.
So there are a number of steps the orthotist should take to ensure a comfortable fit: the patient’s heel should fit fully into the heel cup without excess space, the contours of the plantar surface of the AFO should match the patient’s foot, for children there needs to be up to half an inch growth room in the toe shelf length. At LOC we use our Gait Laboratories at our Kingston and Manchester clinics to fine-tune our bespoke orthotics.
A GRAFO is used to control instabilities in the lower limb by maintaining proper alignment of limbs and controlling their motion. It reaches around to the front of the knee extending down to the ankle. It works by altering a patient’s limb presentation to displace load and impact as well as offering further control to the knee.
The cost of an AFO is dependent on the type of AFO that has been prescribed and the material that it has been made with. Carbon fibre will be more expensive than metal or plastic for example. LOC’s bespoke AFOs cost can be found on our Orthotic Prices page.
The ability to drive while wearing an AFO is dependent on the condition being treated and the orthosis that has been prescribed. If wearing a hinged AFO, for example, you will be able to drive, but if wearing a knee brace, you won’t. Your orthotist will advise you.
The most flexible type of AFO is a Dynamic Ankle Foot Orthosis (DAFO). It is thin and provides flexible support to the foot and ankle.
Both normal AFOs and DAFOs improve static balance (eg: while standing). Research among MS sufferers suggests that DAFOs aided balance while walking more than AFOs.
The simple answer is: yes they can. However one has to be sensible and look for wide-fitting trousers/jeans preferably of light and thin material.
Typically an AFO is stiff and rigid whereas a DAFO is thin, flexible and wraps around the patient’s entire foot. A DAFO provides support but also allows some range of normal movement.
A Supra Malleolar Orthosis SMO gets its name from the part of the body it encompasses. Thus an SMO supports the leg just above the ankle bone or malleoli. It allows dorsiflexion and plantar flexion(toes up and toes down) but eliminates mediolateral movement.
It typically takes a few weeks but is slightly dependent on the chosen materials and current availability.

Sofia’s AFOs Help Her to Stand and Walk During Lockdown

LOC’s gait lab has helped Lilac to move independently

Sam Walmsley to explain OSKAR Framework to Neuro Conference 2021 Delegates

Meet John Turner – our Manchester Orthotics Lead

LOC to launch OSKAR Framework to CMSUK 2020 Delegates

OSKAR Clinic AFOs and gait laboratory are game-changers for cerebral palsy patient Austin

Cerebral palsy patient, Sophie, maintains independence during lockdown with LOC’s help