Functional electronic stimulation (FES) uses the body’s existing nerves and muscles to create a desired contraction in the targeted muscle. Patients who have had an upper motor neurone injury, caused by stroke or cerebral palsy, can usually benefit.
FES works by sending an electrical impulse, either along a nerve that is located close to the surface of the skin, or through a muscle. When the impulse is passed through the muscle it causes a contraction. The big advantage of FES is that it uses the body’s existing muscular system to cause movement and control it; this means that an individual’s muscle strength can be increased or, at least, maintained.
There are also possible benefits to the sensory system. There is some evidence to suggest that FES can assist remyelination in conditions such as multiple sclerosis, or that it improves control by sending signals to the brain. Research is being carried out to validate this.
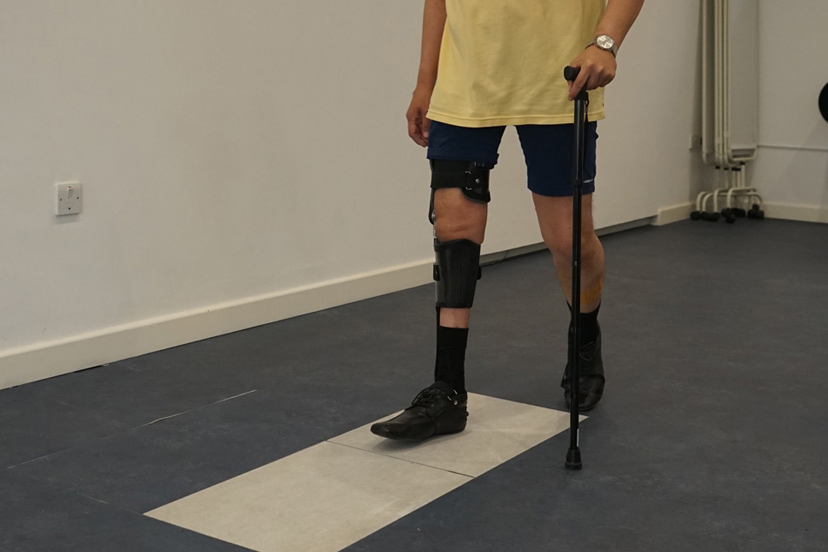
Above: Patient being assessed upon a pressure sensor within LOC's Gait Lab
At the initial consultation, an in-depth history of a patient’s neurological condition will be established. Range of movement, alignment and existing muscle power will be analysed while video gait analysis will study any areas of weakness in slow motion.
If a LOC clinician considers that an individual’s condition is appropriate for FES, then we will test the MyGait system. This involves applying electrodes to targeted areas of the body in order to create the desired muscle contractions. As anatomy can vary between individuals finding the perfect position for the electrodes can take some time. Your clinician will then test the signal from the electrodes and fine-tune the type of muscle contraction that is required.
Once that has been successful, your clinician will use the system while you are walking. MyGait has very sophisticated software that allows fine-tuning of both the timing and strength of the impulses wirelessly as the patient walks. It is possible to see immediate and remarkable improvements.

We have the following facilities and amenities at our Kingston Upon Thames location:
We also have the Gait Laboratory for orthotics patients and Onsite Manufacturing for speedy turnarounds and adjustments whilst you wait.
An insole is a contoured orthotic device which alters the characteristics and biomechanics of the foot and ankle area. Biomechanics are concerned with mechanical laws and how they affect the living body, especially the musculoskeletal system.
They are removable devices, often made from plastic, that are designed to fit inside a shoe to provide additional support for your feet. As well as offering shock absorption, an insole can help distribute the weight of your body more effectively across the foot and can be made bespoke to cover a range of biomechanical conditions.
If you have symptoms in your feet, ankles, hips or your lower back that are intermittent or were not there to start with in early life, and have started to cause you pain over a period of time, bespoke orthotic insoles could be an excellent option.
If you have already tried rest, icing, compression and elevation and your feet have not recovered, we recommend a biomechanical assessment to consider the possibility of insoles. They are a non-invasive approach to treatment and in many cases, are a great option for symptoms that are not severe enough to warrant surgical intervention. Alternatively, they can be considered as an option prior to surgery.
We will send patients away when an insole is not appropriate, if a patient is suffering with iliotibial band syndrome for example, the problem can be helped with physiotherapy and a stretching programme. That’s what our biomechanical assessment is all about; determining whether there would be any benefit from altering the alignment of your feet.

Among 14 to 17-year-old cricket players, there is an increased risk of pars stress fracture, or spondylolysis, which can cause lower back pain and reduced mobility. These athletes are at high risk due to their still-developing bones, which struggle to cope with the repetitive stress of fast bowling.

Apprentice orthotist Catherine Hendy’s journey into the world of prosthetics and orthotics began in an unconventional way. After completing a degree in art, she then trained as an orthotics technician, before taking up an apprenticeship to become a clinician. Now, she’s been nominated for the British Association of Prosthetists and Orthotists (BAPO) Student of the Year 2024.

Amelia was diagnosed with tightness in her neck by her GP before her plagiocephaly diagnosis. Clinician Jo Drake treated her with a LOCband Lite cranial remoulding helmet, which improved her overall head shape and asymmetry.

What are lower limb orthotics, and how can they improve mobility and reduce pain? We've put together this summary of the different kinds of lower limb orthotics, from AFOs and KAFOs to more complex orthotics like RGOs, and how they can help patients with their mobility goals.

Barney's very severe flat head syndrome (plagiocephaly) and diagnosis of torticollis led to successful helmet therapy with the LOCband, significantly improving his head shape, going from 27mm asymmetry to 12mm.

“It’s life-changing, my swimming coach has even remarked what a difference my treatment has made" Read how pectus bracing treatment helped to correct Aris' complex chest deformity, involving a combination of pectus excavatum, pectus carinatum and rib flaring.

Cerebral palsy patient Lucas sees significant improvement in his walking after only six months in his new custom Ankle Foot Orthoses (AFOs), designed by Professor Saeed Forghany in our Manchester clinic. Hear how a detailed gait analysis and bespoke AFOs significantly improved Lucas's gait and comfort.

Freddie’s positional plagiocephaly was treated successfully with the LOCBand Lite, going from 11mm to 2mm after four months in his helmet.