01 June 2023
Scoliosis is a condition where the spine becomes curved and twisted. Approximately three to four in every 1,000 children in the UK have some form of scoliosis. It mostly affects children between the ages of 10 and 15 years old and is also more common in females than males.
Scoliosis can affect people of all ages, but it is most commonly diagnosed during adolescence when growth spurts occur. This is known as adolescent idiopathic scoliosis. Scoliosis can also develop in infants or adults due to other underlying conditions.
In the 1980s, the practice of screening for scoliosis in schools was discontinued. Evidence suggests that this has led to delayed diagnosis of adolescent idiopathic scoliosis in the general population. In practical terms, much of the responsibility now falls on parents to identify the early signs of scoliosis.
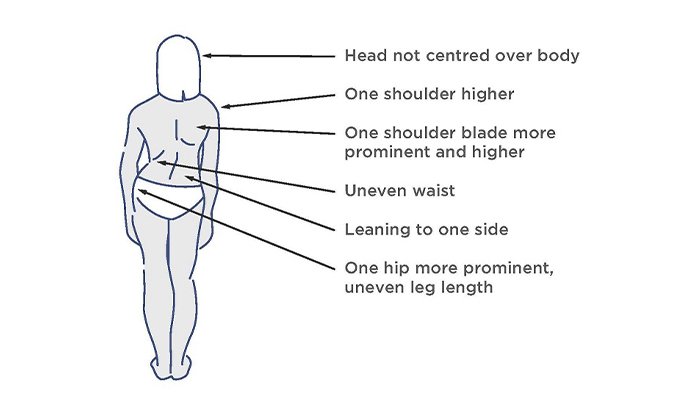
How can you tell if your child has scoliosis? We’ve compiled a helpful guide on what to look out for.
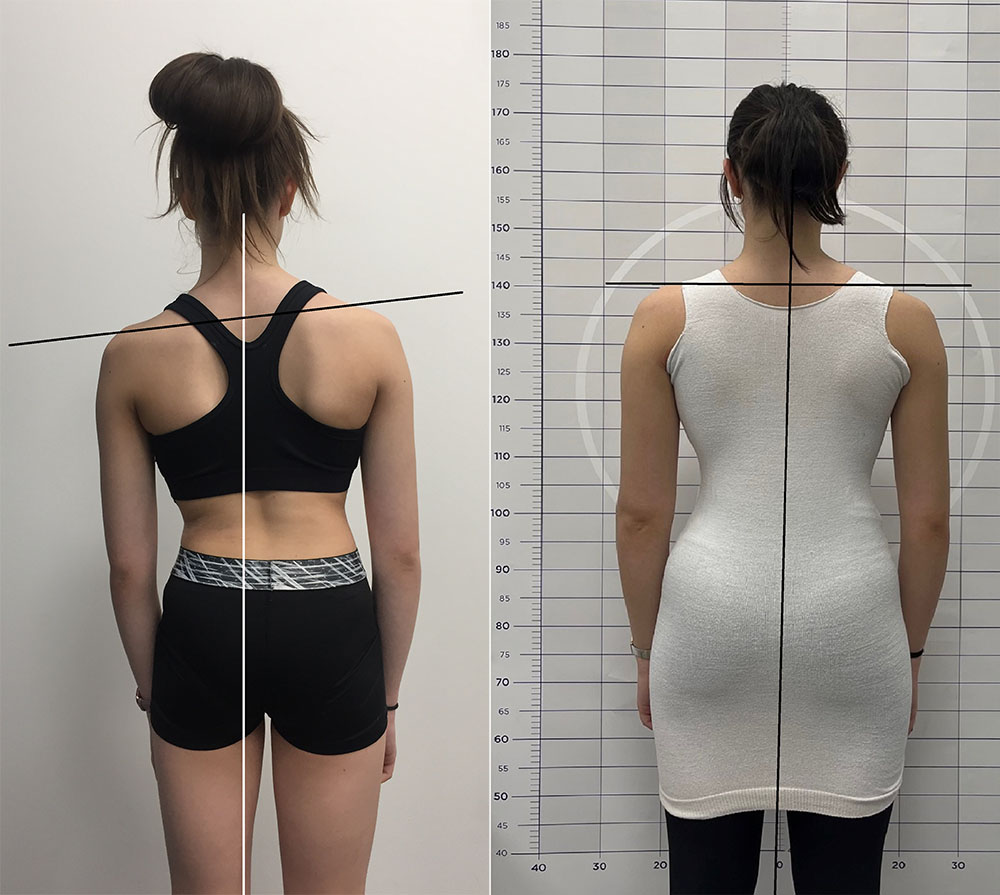
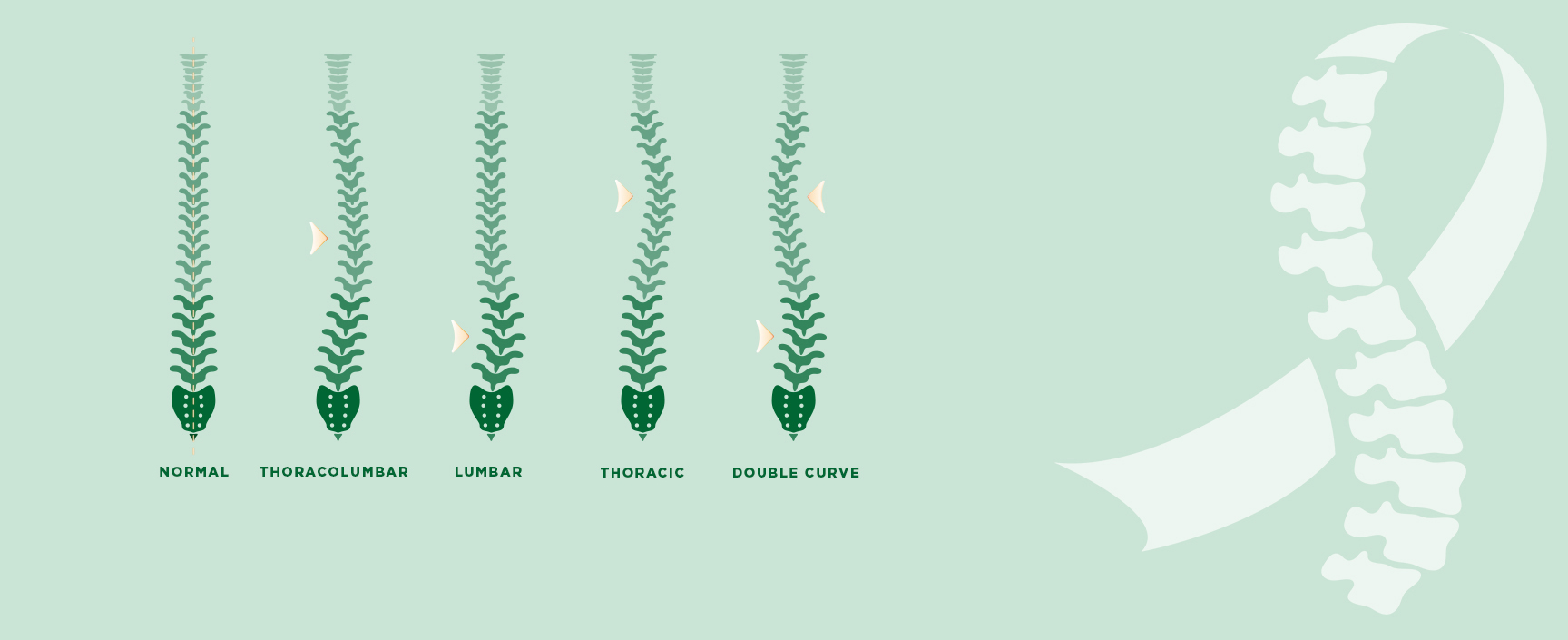
The visual signs of scoliosis include:
Scoliosis awareness and education are essential for parents, teachers, and healthcare professionals. Understanding the signs and symptoms of scoliosis can help in early detection and prompt intervention. All of which can improve the long-term bracing outcomes for individuals with scoliosis.
Scoliosis can progress quickly in adolescence while the skeleton is still growing or during hormonal changes so if you are concerned about your child please contact us.
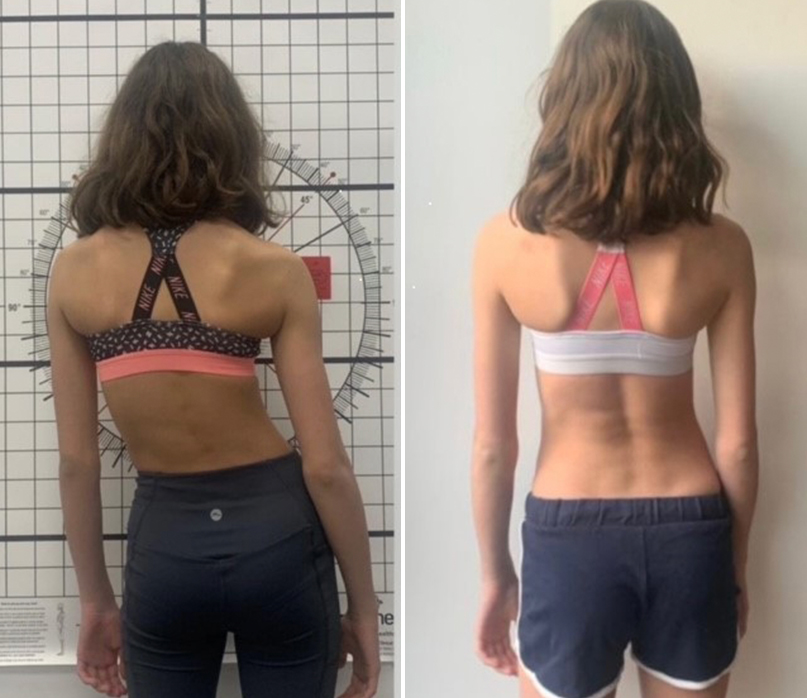
Adolescent Idiopathic Scoliosis patient before and after bracing treatment at LOC.
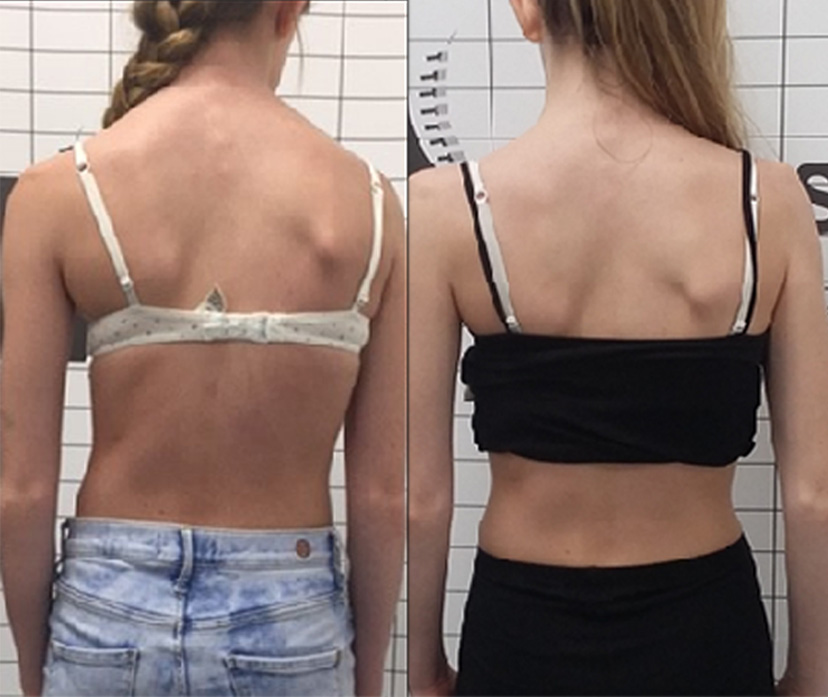
Another adolescent scoliosis patient displaying the visual signs of scoliosis on the left, and showing an improvement after bracing treatment on the right.
We've Got Your Back - Embracing Scoliosis Awareness Month at LOC
We offer a free initial virtual scoliosis consultation for those seeking scoliosis treatment. This initial free virtual consultation can be carried out through Skype, Facetime or Zoom.
This will give you the opportunity to talk directly to one of our specialist clinicians about your child’s scoliosis. During this 15-minute appointment, your clinician will be able to answer any detailed questions or concerns you might have prior to booking a face-face assessment with us.
Find out more information about the LOC Scoliosis Brace
If you think your child, adolescent or adult family member has scoliosis, you can contact LOC directly to arrange a consultation at one of our scoliosis clinics.
If your child has recently been diagnosed with scoliosis or you think they are showing signs of the condition, please contact us.
Scoliosis is a condition where there is an abnormal curvature of the spine. It is a three-dimensional condition with deviation of the vertebrae in the sagittal, coronal and transverse planes.
Treatment recommendations are based on the Cobb angle of the patient and the risk of progression. For curves under 20 degrees, we monitor the patient’s curve while the patient undertakes a tailored exercise programme based on Schroth principles; this is delivered by our partner in providing scoliosis treatment, Scoliosis SOS.
For curves above 20 degrees, we prescribe our LOC Scoliosis Brace which works three-dimensionally to guide the patient’s spine into a more correct position, substantially reducing their Cobb angle. For optimum correction, we recommend that bracing is combined with specialist physiotherapy.
This joint approach means our patients are getting the best and most appropriate advice from two scoliosis specialists, one with an orthotic perspective and one with a physiotherapy perspective.
LOC makes the vast majority of orthotics we fit, and our scoliosis brace is no exception. It is difficult to over-emphasize how important it is to have our own manufacturing unit on site. Lead times are shorter because we are not reliant on outside suppliers, and we can fine-tune our braces at the fitting stage to ensure optimum efficacy and comfort.
The LOC Scoliosis Brace is a 3D, hypercorrective, Cheneau-Gensingen derivative brace, known as one of the most corrective and modern scoliosis braces available in the UK. It is designed to:
The brace is entirely unique and tailored to the patient’s spinal curve pattern, ensuring optimal skeletal correction while prioritising comfort.
Unlike traditional braces, it opens from the front for easier self-application and maintains a low profile under clothing.
The LOC Scoliosis Brace is worn 22 hours a day (including nighttime) and works in conjunction with Schroth-based therapy for maximum results.
Typically, there is an initial consultation followed by a fitting appointment and then pre- and post-reviews after in-brace x-rays; thereafter reviews every three months until the end of treatment. For the majority of our patients who are adolescents, we believe it is essential that there are regular assessments and reviews to ensure that the brace is fitting well; we will make tiny adjustments to the brace to ensure optimum comfort and optimum correction. We have found that comfort is a major contributor to an individual’s compliance with the prescribed wearing regime. In addition, the close contact between patient and clinician ensures patient motivation resulting in better outcomes at the treatment end.
We are pleased to offer a free-of-charge, virtual assessment should you wish to be screened for scoliosis. If we feel a referral to an Orthopaedic Consultant is warranted, we recommend a consultation at The Wimbledon Clinic, Parkside with Mr Darren Lui, Mr Jason Bernard or Mr Tim Bishop. The consultant would arrange the imaging as required. Obviously, you can also seek advice from your family GP.